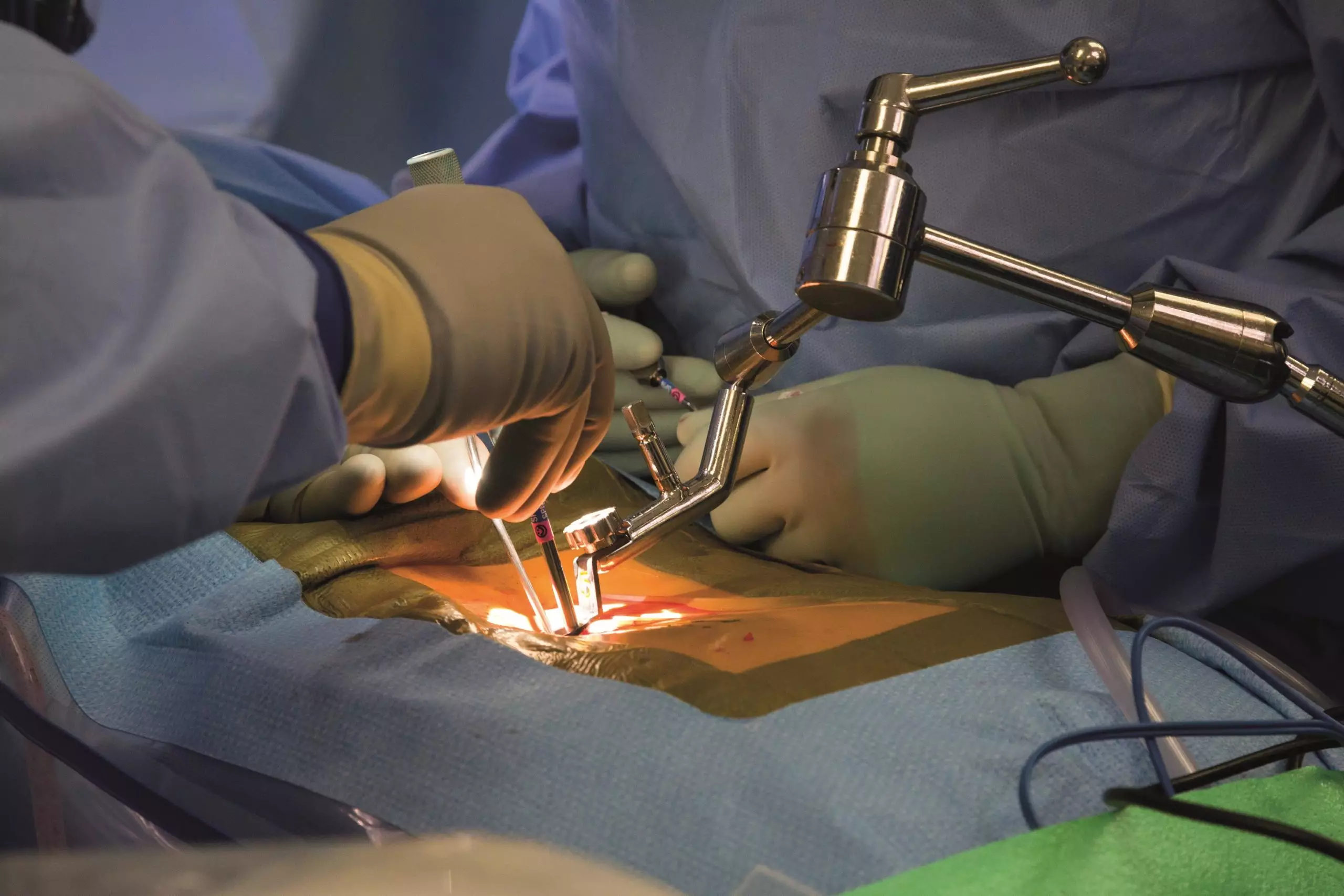
Spinal and Neurosurgery is a multidisciplinary field aimed at protecting the body’s primary support structure and the nervous system that facilitates communication between all organs.
Today, this field encompasses advanced surgical techniques that not only address bone structure abnormalities but also relieve pressure on nerve tissue and provide mechanical stability.
Modern neurosurgical approaches are based on the principle of “functional preservation,” which enables the patient to regain mobility as quickly as possible.
What is Spinal and Neurosurgery? What Conditions Are Treated?
Spinal surgery ensures the safety of this complex pathway through which nerves originating from the brain travel along the spinal canal and branch out to the extremities.
The human spine consists of 33 vertebrae that both enable mobility and protect sensitive nerve tissue.
Any degeneration or trauma in this system can lead to serious consequences for the patient, such as pain, numbness, and even paralysis.
Spinal Anatomy and the Vital Role of the Nervous System
The cervical (neck), thoracic (back), and lumbar (lower back) regions of the spine have different load-bearing capacities and ranges of motion.
The discs between the vertebrae act as suspension, while nerve roots emerge from each level and spread throughout the body.
The primary goal of surgical intervention is to remove mechanical pressure on this anatomy and preserve its dynamic structure.
Degenerative, Traumatic, and Congenital Spinal Disorders
Calcifications that occur with aging, fractures resulting from accidents, or congenital defects (such as spina bifida) may require surgical intervention.
In addition, spinal infections and metabolic bone diseases also fall within the scope of this specialty.
Microsurgical Approach in the Treatment of Lumbar and Cervical Herniated Discs
A herniated disc occurs when the disc tissue between the vertebrae ruptures and protrudes into the nerve canal, creating mechanical and chemical pressure.
Modern surgery focuses on removing the herniation while causing minimal damage to surrounding tissues.
Lumbar Disc Herniation (Lumbar Disc Herniation) and Non-Surgical Treatment Options
Not all lumbar herniations require surgery; the majority of patients can recover with rest, physical therapy, and medication.
The decision for surgery is made in cases of serious weakness, urinary incontinence, or severe, persistent pain, which we refer to as “red flags.”
Symptoms of Cervical Disc Herniation and Surgical Solutions
Neck herniations manifest as pain in the arms, numbness in the hands, and loss of dexterity.
In surgical intervention, the herniated disc is typically removed through an anterior approach (entering from the front of the neck), and a disc prosthesis or cage is placed in its place.
Faster Recovery Process with the Microdiscectomy Method
Microsurgery is a method performed under high-magnification microscopes, requiring only a 1-2 centimeter incision.
This preserves muscle tissue, minimizes bleeding, and allows the patient to be discharged the day after surgery.
Spinal Curvatures and Deformities (Scoliosis and Kyphosis)
Sideways curvature of the spine (scoliosis) or forward bending (kyphosis) can affect both aesthetics and vital organ functions.
Adult and Adolescent Scoliosis Surgery
Curvatures that occur in children during their growth phase or due to degenerative processes associated with aging can be corrected surgically.
Surgical planning is based on the degree of curvature (Cobb angle) and the patient’s growth potential.
Current Surgical Techniques in Kyphosis (Hunchback) Treatment
Excessive kyphosis, especially that associated with osteoporosis or Scheuermann’s disease, is normalized using modern instrumentation techniques.
The screws and rods used during surgery restore the spine to its anatomical alignment.
Prof. Dr. Erdinç Özek: “The most fundamental factor determining success in spinal surgery is intervening at the right time with the right patient. In a herniated disc surgery, our goal is not only to remove the herniation but also to ensure that the patient returns to their social life pain-free. No matter how advanced technology becomes, the surgeon’s experience and the patient’s compliance with the rehabilitation process are the two main pillars of success.”
Spinal Stenosis and Spinal Slippage (Spondylolisthesis)
With aging, the narrowing of the spinal canal leads to a shortening of the patient’s walking distance and a feeling of heaviness in the legs.
Symptoms of Spinal Stenosis: Difficulty Walking and Leg Pain
Patients often report feeling relief when bending forward and experiencing leg cramps when walking upright.
In surgical treatment, the canal is widened (decompression) to allow the nerves to breathe freely again.
Spinal Fusion Surgery and Stabilization
In cases of spinal displacement, the movement of the vertebrae relative to each other compresses the nerves.
In these cases, titanium screws are used to fuse the vertebrae together, providing complete stability.
Spinal Surgery Comparison Table
| Treatment Method | Purpose of Application | Incision Size | Hospital Stay | Return to Normal Life |
| Microdiscectomy | Lumbar/Cervical Herniated Disc | 1.5 – 2 cm | 1 Day | 1 – 2 Weeks |
| Laminectomy | Narrow Canal | 3 – 5 cm | 2 Days | 3 – 4 weeks |
| Spinal Fusion | Spinal Slippage | Variable | 3 – 5 Days | 2 – 3 Months |
| Scoliosis Surgery | Spinal Curvature | Long Incision | 5 – 7 Days | 3 – 6 Months |
Spinal Cord Tumors and Nerve Compression Surgery
One of the most delicate areas of neurosurgery involves tumors that develop within or around the spinal cord.
Approach to Intradural and Extradural Spinal Cord Tumors
The location of the tumor determines the degree of difficulty of the surgery.
The primary goal is to remove the tumor (total resection) without damaging the nerve tissue using microsurgical techniques.
Peripheral Nerve Surgery: Entrapment Neuropathies and Repairs
In conditions such as carpal tunnel syndrome (wrist) or ulnar nerve compression (elbow), releasing the compressed nerve prevents permanent damage.
Advanced Technologies in Spinal Surgery: Navigation and Neuromonitoring
Advancing technology has minimized the “risk of paralysis” fear, maximizing surgical safety.
Minimally Invasive Spinal Surgery (Closed Procedures)
In these surgeries, performed using small tubes and endoscopes, tissue damage is so minimal that the recovery process is incredibly accelerated.
Nerve Safety During Surgery: The Importance of Neuromonitoring
The patient’s nerve transmissions are monitored in real-time throughout the surgery.
When the surgeon approaches a nerve, the system alerts the surgeon by signaling, thereby enhancing the safety of the operation.
Post-Spinal Surgery Recovery and Physical Therapy Process
The success of the surgery does not end on the operating table; it must be complemented by a proper rehabilitation process.
Early Postoperative Movement and Rehabilitation
In modern protocols, patients are mobilized just a few hours after surgery.
Early mobilization reduces the risk of clots and triggers healing hormones.
Anonymous Case Study
Our 55-year-old patient, who presented with severe leg pain and difficulty walking (spinal stenosis), had a walking distance reduced to 50 meters.
Following micro-decompression and stabilization surgery, the patient was able to walk with a brace on the second day after surgery and returned to their daily routine without pain by the sixth week.
Frequently Asked Questions
What is the risk of paralysis after spinal surgery?
Thanks to the neuro-monitoring technology and microsurgical techniques used today, the risk of nerve damage has been reduced to less than 1%; with an experienced surgeon and the right technological infrastructure, this risk is minimized.
Does a herniated disc recur after surgery?
The recurrence rate after a successful microsurgical operation is quite low; however, if the patient does not pay attention to their weight, lifts heavy objects, and does not follow the principles of back protection, there is a 5-10% risk of recurrence.
Does spinal fusion (implant placement) restrict movement?
Screw fixation is only performed to stabilize areas with slippage or loss of stability; with modern techniques, only the problematic segment is targeted, so the patient does not experience significant limitations in general bending and twisting movements.
How soon after surgery can I start walking?
In most surgeries performed using microsurgery or minimally invasive techniques, patients are mobilized approximately 4 to 6 hours after the operation and discharged the next day.
Can scoliosis surgery be performed at any age?
Although scoliosis surgery is more commonly performed during childhood and adolescence, thanks to advances in technology, it can also be safely performed on adult and elderly patients with degenerative scoliosis, improving their quality of life.
Does herniated disc surgery affect sexual life?
Severe pressure on the nerves caused by the herniation can lead to sexual dysfunction; surgical intervention helps preserve function by relieving this pressure, and patients can return to normal life after the recovery process.
Prof. Dr. Erdinç Özek
“Most of my patients delay surgery due to fear of paralysis. However, it should not be forgotten that irreversible damage to a compressed nerve is much greater than the risk of surgery. Using the possibilities offered by technology, an intervention performed within safe limits is life-saving.”
For early diagnosis and proper planning regarding your spinal health concerns, you can consult with a specialist.
You can schedule an appointment at our clinic in Istanbul to determine the suitability of surgery for your condition and the most appropriate method for you.
Scientific References
European Spine Journal: “Microsurgical versus open discectomy for lumbar disc herniation” (Comparison of microsurgery and open surgery for lumbar disc herniation).
https://link.springer.com/article/10.1007/s00586-014-3674-x
Journal of Neurosurgery (Spine): “Intraoperative neuromonitoring in spine surgery: A state-of-the-art review.”
https://thejns.org/spine/view/journals/j-neurosurg-spine/26/1/article-p1.xml
PubMed / NCBI: “Minimally invasive spine surgery: Technical nuances and clinical outcomes.”
https://pubmed.ncbi.nlm.nih.gov/31333148/
The Lancet Rheumatology: “Global, regional, and national burden of low back pain” (Worldwide burden of low back pain and incidence data).
https://www.thelancet.com/journals/lanrhe/article/PIIS2665-9913(23)00098-X/fulltext