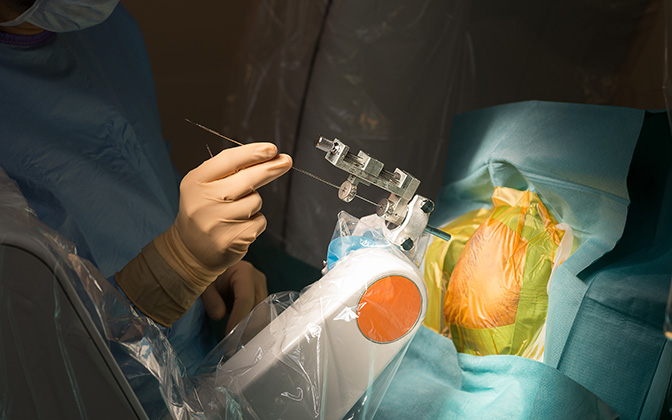
Functional brain surgery is one of the most dynamic fields of neurosurgery, aiming to treat conditions where the nervous system appears structurally normal but is functionally impaired.
This branch re-regulates nerve transmission through surgical or electrical methods in cases of movement disorders, chronic pain, and epilepsy that do not respond to drug treatment.
In modern medicine, these approaches focus on improving quality of life by “modulating” faulty signal loops in the brain rather than altering the patient’s anatomical structure.
What is Functional Brain Surgery? Which Diseases Are Treated?
Functional neurosurgery is the art of regulating abnormal electrical activity by intervening in specific areas of the brain.
The difference from traditional brain surgery is that the focus is not on removing a tumor, but on restoring the brain’s network.
This discipline combines microsurgical techniques and advanced technology to help patients regain their independence in daily life.
Restoration of Nervous System Functions and Quality of Life-Focused Approach
The treatment philosophy is based on the principles of “repair” and “balancing.”
Excessive activity or transmission deficiencies in neural circuits are detected using advanced technologies and addressed accordingly.
Symptoms such as tremors, spasms, and seizures are controlled through this restoration process.
Basic Pathologies Covered by Functional Neurosurgery
This surgical field addresses a wide range of neurological disorders:
Parkinson’s disease and dystonias.
Essential tremor (familial tremor).
Drug-resistant epilepsy cases.
Spasticity (severe muscle stiffness).
Chronic pain syndromes such as trigeminal neuralgia.
Surgical Solutions for Movement Disorders: Parkinson’s and Dystonia
Movement disorders are one of the most significant neurological disabilities that limit a patient’s physical independence.
When medications are insufficient or cause serious side effects, functional brain surgery comes into play.
What is Deep Brain Stimulation (DBS – Brain Pacemaker)?
Deep Brain Stimulation (DBS) is a procedure that involves delivering continuous electrical stimulation to the brain through electrodes implanted deep within the brain.
Commonly known as the “brain pacemaker,” this method suppresses the brain centers producing faulty signals to control symptoms.
DBS differs from other surgical methods because it is reversible and adjustable.
Neuromodulation in Essential Tremor and Tremor Disorders
In patients with essential tremor, especially hand tremor, it can lead to social isolation and difficulty eating.
Thanks to neuromodulation applied to the thalamus region, tremors can be reduced by 80-90%.
This intervention allows patients to regain basic skills such as writing or drinking a glass of water.
Suitable Candidates for Parkinson’s Surgery and the Evaluation Process
Not every Parkinson’s patient is suitable for surgery.
Ideal candidates are those who initially respond well to medication but over time experience a decrease in the medication’s effectiveness or the onset of the “on-off” phenomenon.
Detailed neuropsychological tests and MRI studies are conducted before surgery to analyze the chances of surgical success.
Prof. Dr. Erdinç Özek: “Functional surgery is not a matter of hope, but a mathematical and physiological planning process. Success in Parkinson’s surgery depends not only on the electrode being placed in the correct millimeter, but also on the patient’s psychological readiness and the meticulous adjustment of the battery after surgery. My biggest advice to our patients is to seek expert opinion before symptoms completely destroy their quality of life.”
Drug-Resistant Epilepsy (Sara) Surgery and Treatment Protocols
In approximately one-third of epilepsy patients, medications cannot control seizures.
In such cases, surgical options are the most effective way to reduce the frequency and severity of seizures.
Epilepsy Stimulator (Vagal Nerve Stimulation – VNS) Application
In cases where brain intervention is risky, a pacemaker (VNS) implanted in the vagus nerve in the neck is preferred.
This device sends regular signals to the brain, raising the seizure threshold and shortening the duration of seizures.
Resective Surgery: Surgical Removal of Seizure Foci
If seizures are determined to originate from a single lesion in the brain, surgical removal (resection) of this area can completely eliminate seizures.
Advanced imaging techniques are used during this process to avoid damaging healthy brain tissue.
Functional Interventions in the Management of Spasticity and Chronic Pain
Severe muscle spasms (spasticity) that develop after brain or spinal cord injury make patient care difficult and cause pain.
Baclofen Pump (Intrathecal Baclofen Pump) and Muscle Rigidity Treatment
Taking high doses of muscle relaxant medications orally can cause side effects.
The baclofen pump delivers the medication directly into the spinal fluid, providing maximum relaxation with very low doses.
This method significantly increases comfort even in bedridden patients.
Surgical Intervention Methods for Trigeminal Neuralgia and Facial Pain
In trigeminal neuralgia, also known as “suicide pain,” the blood vessel pressing on the facial nerve is separated using microsurgery (Microvascular Decompression).
This procedure can provide immediate relief from the patient’s chronic severe pain.
Functional Brain Surgery Comparison Table
| Treatment Method | Target Disease | Application Method | Recovery Period | Decision Criteria |
| Deep Brain Stimulation (DBS) | Parkinson’s Disease, Dystonia, Tremor | Intracerebral electrode + Subcutaneous battery | 2-4 weeks | Drug side effects / Non-response |
| Vagus Nerve Stimulation (VNS) | Drug-resistant epilepsy | Neck region nerve stimulation | 1 week | Focal seizures |
| Baclofen Pump | Spasticity, MS, Cerebral Palsy | Abdominal pump placement | 2-3 Weeks | Severe muscle spasms and pain |
| Microvascular decompression | Trigeminal Neuralgia | Posterior cranial microsurgery | 3-4 weeks | Facial pain that does not respond to medication |
How is Functional Brain Surgery Performed? The Surgical Process and Technology
The surgical process requires millimeter-precise calculations and advanced technological equipment.
Brain mapping techniques are used during surgery to minimize the margin of error.
Stereotactic Methods and Microelectrode Recording System
In DBS surgeries performed while the patient is awake, electrical signals from the brain are monitored.
Thanks to the microelectrode recording system (MER), the exact coordinates of the targeted cell group are verified.
This ensures that the electrode is placed at the most effective point.
Neuronavigation and Intraoperative Imaging-Assisted Planning
Neuronavigation guides the surgeon’s journey within the brain like a GPS system.
High-resolution MRI and CT images taken before surgery are integrated into surgical robotic systems.
Postoperative Recovery and Follow-up in Functional Neurosurgery
The success of the surgery depends as much on the postoperative follow-up process as on the surgical intervention itself.
Pacemaker Settings (Programming) and Long-Term Functional Gains
In the first few weeks after the brain implant is placed, the ideal frequency and voltage settings are adjusted based on the patient’s symptoms.
These settings are optimized for each patient using remote control devices.
Patients are brought to the best clinical outcome with the lowest possible medication dose through regular check-ups.
Anonymous Case Experience
A 62-year-old Parkinson’s patient was unable to walk daily despite increasing medication doses.
Following bilateral subthalamic nucleus (STN) DBS surgery, the patient’s tremors decreased by 85%.
Six months after the surgery, the patient was able to perform daily activities without the use of assistive devices, and the medication dose was reduced by half.
Frequently Asked Questions
Is brain pacemaker surgery risky?
Thanks to modern neuronavigation and imaging techniques, the risks are quite low; as with any surgical procedure, there is a possibility of infection or bleeding, but this risk is minimized by experienced hands and technological equipment.
Is there an age limit for Parkinson’s surgery?
The patient’s overall health, cognitive functions, and presence of additional diseases are more decisive factors than calendar age when deciding on surgery; however, patients under the age of 75-80 are generally considered more suitable candidates.
What is the lifespan of a brain pacemaker?
Depending on the voltage settings used, non-rechargeable batteries generally last between 3 and 5 years, while rechargeable new-generation batteries can last up to 15 to 25 years.
Does being awake during surgery cause pain?
The patient does not feel pain because the scalp and bone tissue are completely numbed with local anesthesia; the purpose of keeping the patient awake is to instantly test speech and movement functions while placing the electrodes to find the most accurate point.
Are medications completely discontinued after epilepsy surgery?
Although the goal is for seizures to stop completely after surgery, the decision to discontinue medication is not made immediately; medication doses can be gradually reduced over months under specialist supervision, based on the patient’s clinical course and EEG results.
Can an MRI be performed after a brain pacemaker is implanted?
The vast majority of new-generation stimulator systems are manufactured as “MRI-compatible” (MR Conditional); however, it is mandatory for the stimulator to be set to the appropriate mode by the technical service or your doctor before the scan.
When will the effects of the surgery begin to be seen?
In procedures such as DBS, symptoms such as tremors may improve immediately after the stimulator is turned on and correctly programmed; however, full clinical stabilization is achieved within the first few months as the stimulator settings are optimized.
Prof. Dr. Erdinç Özek: “The change in the patient’s life after functional surgery sometimes happens overnight. However, it is important to remember that this process is a marathon. The communication bridge between the surgeon, neurologist, and patient is the most important factor determining the lasting success of the treatment.”
You can consult an expert to obtain comprehensive information about functional brain surgery and modern treatment protocols and to assess whether your condition is suitable for surgery.
You can start your neurological and surgical evaluation process by scheduling an appointment at our clinic in Istanbul.
Scientific References
The New England Journal of Medicine (NEJM): “A Randomized Trial of Deep-Brain Stimulation for Parkinson’s Disease”.
The Lancet Neurology: “Efficacy and safety of thalamic deep brain stimulation in essential tremor”.
Journal of Neurosurgery (JNS): “Long-term outcomes of vagus nerve stimulation in drug-resistant epilepsy”.
Movement Disorders Journal: “Guidelines for the surgical treatment of Parkinson’s disease”.
PubMed / NCBI: “Microelectrode recording in functional neurosurgery: Techniques and clinical impact”.