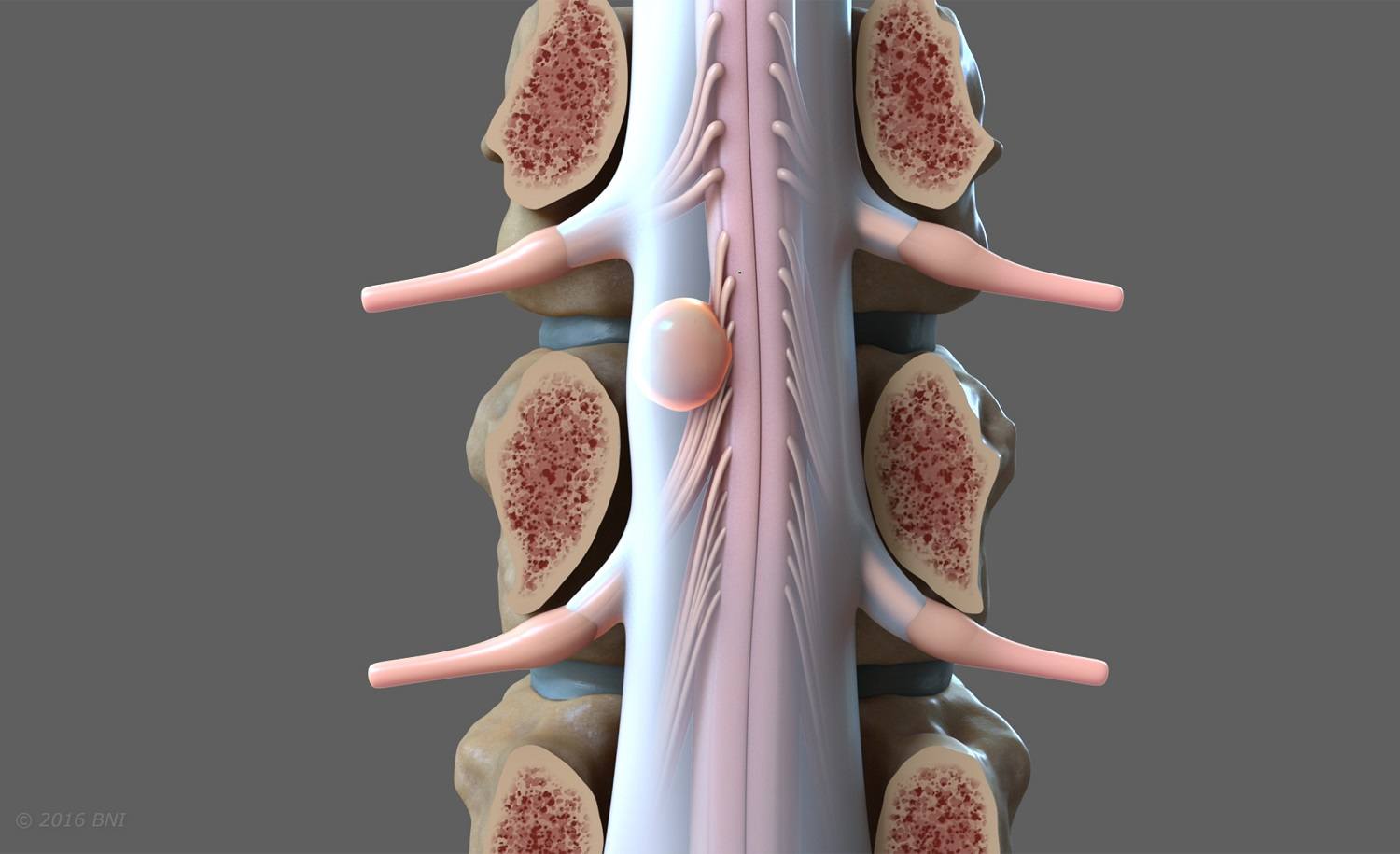
Brain and spinal cord tumors are serious health conditions that require a multidisciplinary approach due to the complex structure of the central nervous system. Neuro-oncology is the field of expertise that covers the diagnosis, surgical intervention, and post-surgical treatment processes of these masses.
What is Neuro-Oncology? Brain Tumor Treatment in Adults
Adult neuro-oncology deals with the management of tumors originating from the brain’s own tissue (primary) or spreading from other organs (metastatic).
Glioblastoma: Originates from the brain’s supporting tissue. Surgery is the cornerstone of oncological treatment for aggressive types such as glioblastoma.
Meningiomas: These are masses originating from the brain membranes, which are generally benign but can put pressure on critical blood vessels and nerves.
Brain Metastases: Especially in cases of lung and breast cancer spreading to the brain, surgical intervention may be necessary to reduce the mass effect and improve quality of life.
Pediatric Neuro-Oncology: Childhood Brain Tumors
Childhood tumors differ from adult tumors in terms of their biological structure and treatment response. Since the child’s brain is still developing, surgical planning must be extremely precise.
Common Tumor Types in Children
Tumors in the posterior fossa (cerebellum) region are particularly common in children. Medulloblastoma and ependymoma are the most typical examples in this group. Early diagnosis is critical for preventing permanent neurological damage and protecting developmental processes in children.
Neuro-Oncological Surgery and Modern Techniques
The goal in tumor surgery is “maximal safe resection,” which means removing as much of the tumor as possible without damaging healthy tissue.
Surgical Methods and Technology Comparison Table
| Method / Technology | Application Area | Key Advantage | Recovery Time |
| Microsurgery | All Tumor Types | Enables tissue differentiation with high magnification. | 4 – 6 Weeks |
| Neuronavigation | Deeply Seated Masses | Pinpoints the tumor’s location to the millimeter. | 2 – 4 Weeks |
| Awake Craniotomy | Speech/Motor Centers | Provides functional testing during surgery. | 3 – 5 Weeks |
| Endoscopic Surgery | Skull Base/Ventricle | Minimizes incision size and trauma. | 1 – 2 weeks |
Recommendations from Prof. Dr. Erdinç Özek
“Receiving a brain tumor diagnosis can be devastating for patients and their families. However, in modern surgery, we can visualize the tumor’s boundaries using fluorescent dyes (5-ALA) and preserve your speech center through awake surgery. Especially in pediatric cases, surgical success is not only about removing the tumor but also ensuring the child’s continued social and cognitive development. Treatment is a team effort; the joint decision of the neurosurgeon, oncologist, and radiation therapist is the most appropriate approach.”
Clinical Experiences and Case Example
Anonymous Case Analysis: A 7-year-old child presented with complaints of projectile vomiting in the mornings and unsteady gait. An MRI scan revealed a mass (suspected medulloblastoma) obstructing the fourth ventricle in the cerebellum. During the microsurgical operation performed by Prof. Dr. Erdinç Özek, 98% of the mass was successfully removed with neuromonitoring. After the surgery, the patient’s cerebrospinal fluid flow returned to normal, and the patient was discharged without neurological loss and referred to the necessary oncological treatment process.
Multidisciplinary Treatment Approach
Once the postoperative tissue diagnosis (pathology) is confirmed, the treatment process is not considered complete. Through Tumor Boards, the necessity of radiotherapy or chemotherapy is evaluated based on the patient’s age and the tumor’s genetic characteristics. In pediatric patients, much more precise dose planning is performed, taking into account the effects of radiotherapy on development.
Frequently Asked Questions
Is brain tumor always treated with surgery?
Not every mass requires surgery; depending on the type, location, growth rate, and symptoms of the tumor, some cases can be monitored with radiosurgery or close follow-up alone.
Are childhood brain tumors different from those in adults?
Tumors in children differ in terms of biological behavior, location, and response to treatment; therefore, pediatric cases require special surgical strategies that protect the developing brain tissue.
Should benign brain tumors be surgically removed?
Although benign masses are not cancerous, they can cause neurological deficits or seizures by pressing on brain tissue as they grow, so surgical removal is recommended once they reach a certain size.
Does personality change occur after brain tumor surgery?
Changes may be seen when the tumor affects behavioral centers such as the frontal lobe of the brain; however, surgical intervention generally aims to preserve function by relieving this pressure.
Does surgery ensure complete removal of the tumor?
With the help of microsurgery and neuronavigation, most of the tumor can be safely removed; however, additional treatments such as radiotherapy or chemotherapy may be applied after surgery for microscopic residues.
How long is the hospital stay after brain tumor surgery?
Depending on the extent of the surgery, patients are generally kept under observation in the hospital for 3 to 5 days after surgery before being discharged.
Detailed Information and Expert Opinion
Neuro-oncological diseases require careful follow-up and high surgical expertise. For professional information about the surgery of adult and childhood brain tumors, you can contact Prof. Dr. Erdinç Özek’s clinic. You can request a detailed evaluation about modern medical approaches by making an appointment at our center in Istanbul.
Scientific References
Journal of Neuro-Oncology: Standard of care in adult glioblastoma management. https://link.springer.com/journal/11060
The Lancet Child & Adolescent Health: Current perspectives on pediatric medulloblastoma. https://www.thelancet.com/child-adolescent
PubMed (NIH): Intraoperative neuromonitoring in pediatric neurosurgery. https://pubmed.ncbi.nlm.nih.gov